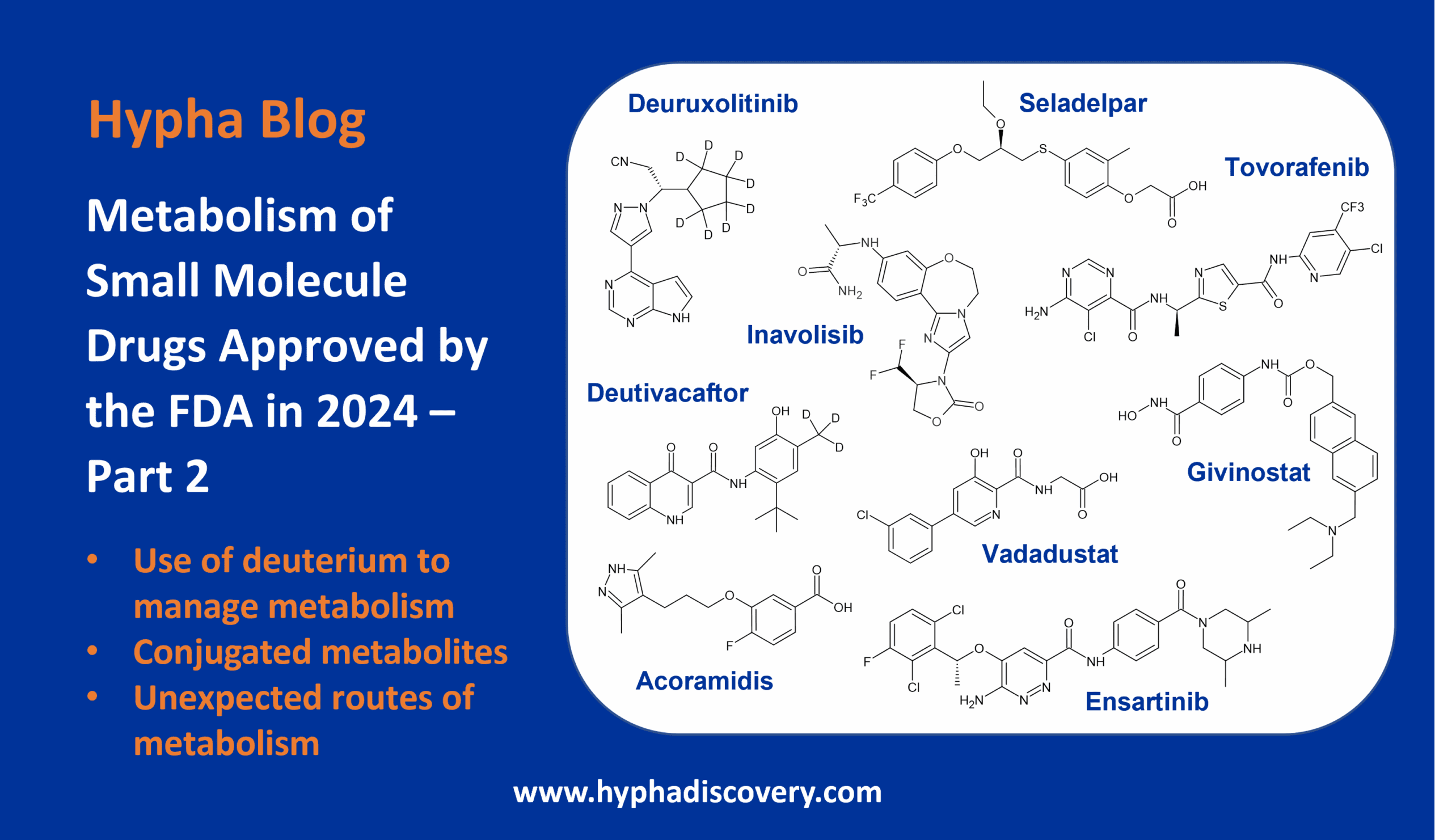
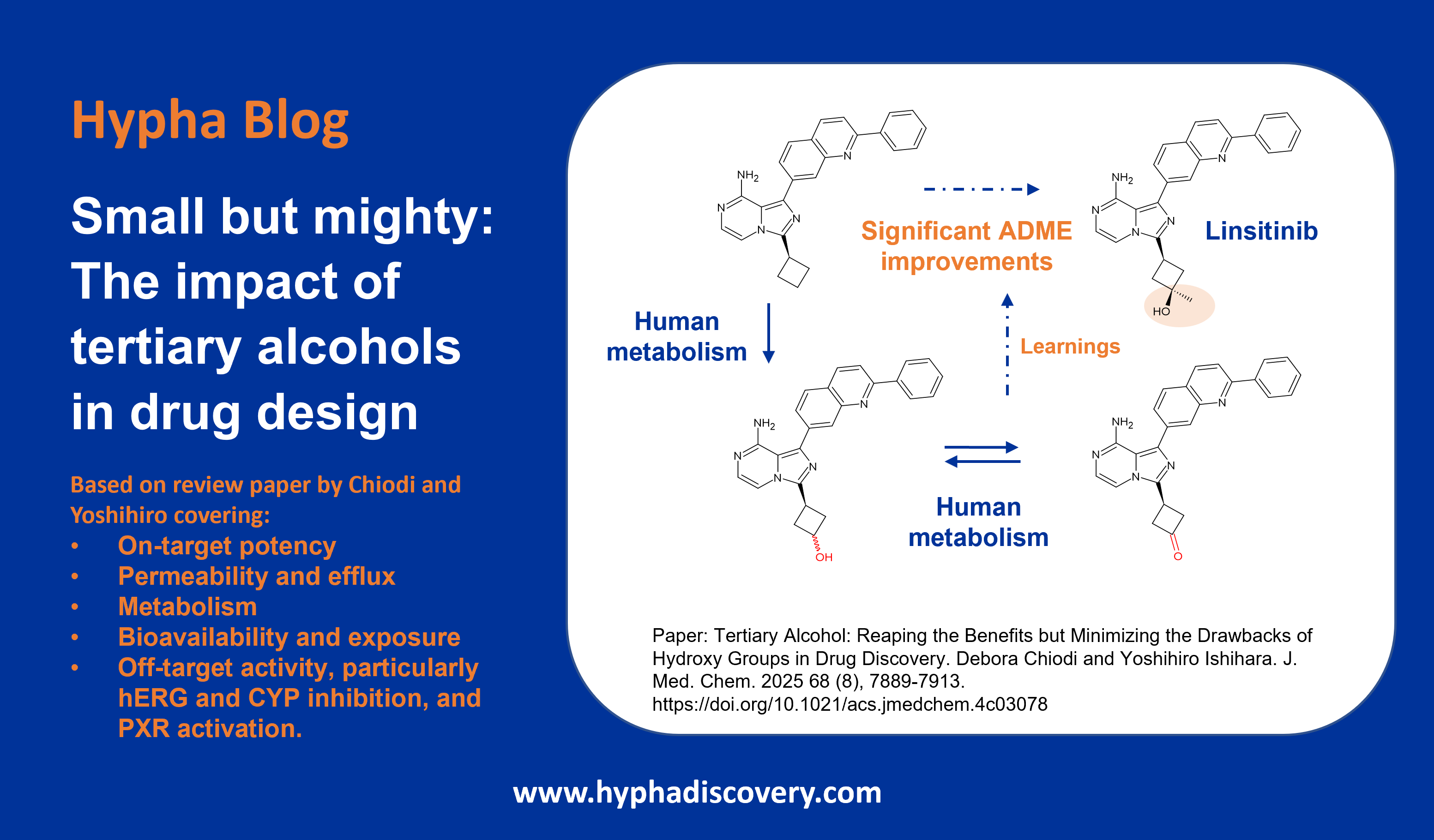
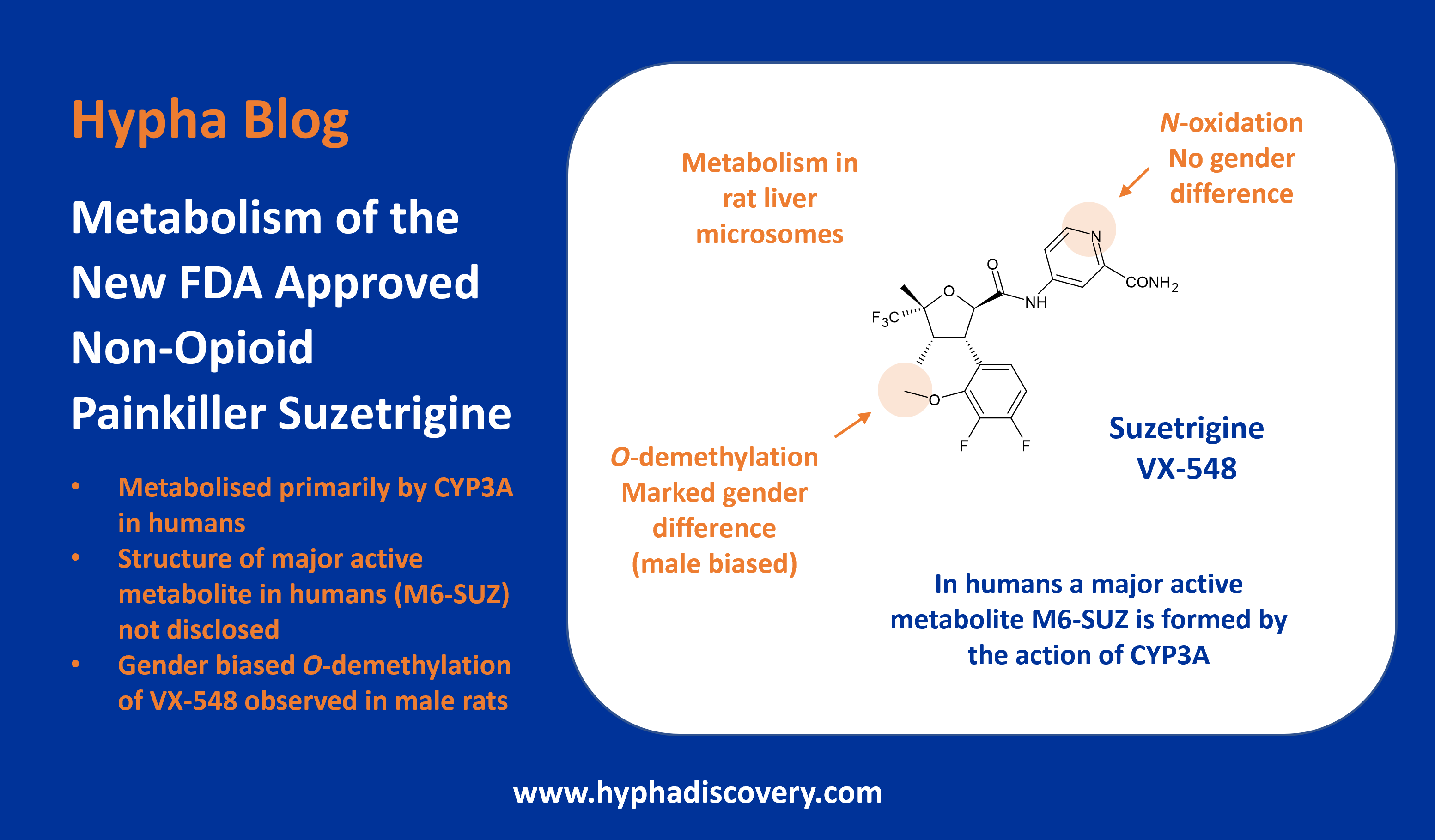
Breaking C-F bonds in drugs – metabolism mediated release of fluorine
By Samuel Coe and Julia Shanu-Wilson

Lenacapavir, recently approved for multi-drug resistant HIV-1 infection, contains 10 fluorine atoms.
Fluorine is a highly reactive chemical element that has a unique electron configuration and provides valuable benefits in medicinal chemistry. Increasingly used in drug design, some drug structures are now bristling with fluorine atoms.
Fluorine is unique in its ability to positively impact on several important properties, including pKa, biological activity, lipophilicity and, crucially for the medicinal chemist, metabolism. Since fludrocortisone, the first fluorine-containing drug, was brought to market in 1954, there has been a dramatic rise in the number of drugs containing fluorine [1]. Now >20% of all commercialised medicines in the pharmaceutical industry contain a fluorine atom [2]. This is no doubt linked to the advances in chemical synthesis tools for installing F that are milder and with wider application than just deoxyfluorination [3].
Although fluorine-containing organic compounds are rare in nature, incorporation of fluorine into drug scaffolds is common and spans therapeutic classes. In 2021, almost one third of FDA approved drugs contained at least one fluorine. In 2022, fewer of the 19 newly FDA approved small molecule drugs contained F atoms (adagrasib, lenacapavir, oteseconazole, vonoprazan), but this was followed by 3 more approvals of F-containing drugs in the first quarter of 2023 alone (pirtobrutinib, omaveloxolone, leniolisib). Even newer from the pharma benches are 12 small molecule drugs highlighted by Chris de Savi [4], whose structures were first disclosed at the ACS and AACR meetings in Q1 2023. Of these 12 drugs, 9 contain at least one fluorine!
Homolytic cleavage of the C-F bond requires very high input of energy (109 kcal/mol) compared to the C-H bond. This has made fluorine a go-to tool for mitigating metabolic soft spots in aliphatic and aromatic moieties. However, this chemically robust bond is not impenetrable. Indeed, under physiological conditions the C-F bond is cleaved heterolytically; the release of F being facile with certain nucleophiles or the action of metabolising enzymes [5].
The menace of free fluorine
Voriconazole
The release of fluorine from drugs can cause high plasma fluoride levels leading to periostitis – inflammation of the periosteum resulting in skeletal pain. Although the exact relationship remains unclear, excess fluoride intake has been proposed as a cause of voriconazole-related periostitis. Each voriconazole molecule contains three fluorine atoms and 5% of the dose is estimated to be metabolized via CYP2C19 to generate free fluoride. Fluoride ions have a similar size and electrical charge to hydroxyl ions but greater affinity for calcium, resulting in fluorapatite replacing hydroxyapatite in the bone matrix, stimulating excess bone formation [6].
Oxidative defluorination and hepatotoxicity
Like gefitinib and famitinib, oxidative defluorination has been shown to result in a reactive intermediate implicated in idiosyncratic hepatotoxicity during the metabolism of the tyrosine kinase inhibitor sunitinib. Serious enough that sunitinib carries a boxed warning.
Although the major route of metabolism of sunitinib is via CYP3A4 mediated N-deethylation to an active metabolite M1, CYP1A2 (and to a lesser extent CYP3A4/5 and CYP1A1) catalyse the metabolic activation of sunitinib to defluorinated sunitinib (M3), from which a reactive quinoneimine is formed, resulting in trapping of a GSH conjugate (M5) and generation of a cysteine conjugate (M6) [7,8].

Figure 1: Oxidative defluorination of sunitinib to reactive metabolites [adapted from Scheme 1 in ref 8]
PET tracer defluorination
Defluorination in vivo has also been observed in some organofluorosilicon PET tracer candidates where CYP2E1 metabolic biotransformation led to the detachment of the radiolabel, with hydroxylation of the tert-butyl group adjacent to the silicon, followed by oxidative defluorination cleaving the fluorine off the silicon [9].
We now take a look at some other key examples that highlight motifs and scaffolds that could release toxic fluorine metabolites after bioactivation.
Eliminating HF and Michael Acceptors
Metabolism of some alkyl fluorides can generate an acidic group neighbouring the fluorination site, which following deprotonation may release fluoride and form a Michael acceptor.

Figure 2 Initial lead compound and attenuation of metabolic liability through introduction of a methyl group in the azepane ring α to the primary amine [10]
The PIM kinase inhibitor illustrated in Figure 2 contains a difluorinated azepane, where the fluorine groups played a critical role in the formation of reactive metabolites. GSH trapping supported the generation of a Michael acceptor through an oxidative cleavage of the amine and HF elimination, which could then covalently react with CYP3A4 [10]. Clever use of truncated tool compounds with fewer sites susceptible to biotransformation enabled quick probing of the culprit pharmacophore. Subsequent addition of a methyl group α to the primary amine prevented oxidation and resulted in elimination of CYP3A time dependent inhibition (TDI).
Location Location Location

Figure 3 Installation of fluorine in the piperidine ring to avoid toxicity that resulted from metabolic release of fluoroacetate on the piperidine nitrogen [11]
Fluorine is commonly used to attenuate the basicity of nitrogens in drug molecules. During the development of a series of kinesin spindle protein inhibitors, this property was used to modulate the basicity of a piperidine nitrogen [11]. The most advanced fluorine-containing compound at the time contained a fluoroethylamine on the piperidine nitrogen but was unfortunately metabolised via N-dealkylation, releasing the known toxin fluoroacetate as a byproduct. The result was acute toxicity, causing death in the pre-clinical animal model. To avoid the liability of fluoroethylamine, a fluorine was installed in a metabolically benign location on the piperidine ring, so avoiding toxic metabolite formation.
Interestingly, the stereochemistry of the F in the ring affected the pKa in different ways. The axial fluorine had a modest effect reducing the pKa to 7.6 vs 8.8 of the parent while the equatorial fluorine reduced the pKa to 6.6! A major improvement that had far reaching effects on activity and MDR ratios.
Bioactivation and aromatic defluorination
Although the addition of fluorine to aromatic rings is in principle a simple solution for blocking metabolic soft spots, oxidative defluorination can occur, generating phenols and the release of fluoride. In addition, this can lead to reactive quinone, quinone imine and quinone methide metabolites resulting in TDI of CYPs and GSH adducts [5].
Bioactivation of the fluoropyrimidine moiety of a BACE1 inhibitor lead compound resulted in reactive metabolite formation via oxidative defluorination and was responsible for TDI of CYP3A4 [12]. This was surprising given that replacement of a phenyl with a pyrimidine and fluorination of aryl or heteroaryl rings are techniques often used to increase metabolic stability.

Figure 4 Oxidation of the pyrimidine ring to reactive intermediates results in defluorination and glutathione conjugation, prompting development of a defluorination-resistant analogue [12].
The oxidative defluorination metabolite was hypothesised to be formed by two electron reduction of a quinone iminium intermediate by NADPH mediated by P450 reductase. The substitution of methyl groups at both the 4- and 6-positions of the 5-fluoropyrimidine ring decreased the ability to form epoxide and quinone iminium intermediates, and ameliorated the TDI.
The bigger picture
It should not be forgotten that fluorinated drugs are highly prescribed, and an average patient may take several such drugs at the same time over an extended period. Consequently, potential environmental concerns have been raised, stemming from the detection of metabolically stable fluorinated drugs in surface waters and biological samples, which have been designed to be highly resistant to degradation [13]. This wider environmental concern is interesting to consider as fluorine becomes an even more ubiquitous element in commonly used drugs.
References
[1] Metabolic and Pharmaceutical Aspects of Fluorinated Compounds. Benjamin M. Johnson, Yue-Zhong Shu, Xiaoliang Zhuo, and Nicholas A. Meanwell. Journal of Medicinal Chemistry 2020 63 (12), 6315-6386, https://doi.org/10.1021/acs.jmedchem.9b01877
[2] Synthesis and Applications of Selected Fluorine-Containing Fluorophores. Casa, S.; Henary, M. Molecules 2021, 26, 1160. https://doi.org/10.3390/molecules26041160.
[3] The Fluorination of C-H Bonds: Developments and Perspectives. Szpera R, Moseley DFJ, Smith LB, Sterling AJ, Gouverneur V. Angew Chem Int Ed Engl. 2019 Oct 14;58(42):14824-14848, https://doi.org/10.1002/anie.201814457
[5] The Dark Side of Fluorine. Pan Y. ACS Med Chem Lett. 2019 Jun 20;10(7):1016-1019, https://doi.org/10.1021/acsmedchemlett.9b00235
[6] Voriconazole-Associated Periostitis: New Insights into Pathophysiology and Management. Bennett, M.J., Balcerek, M.I., Lewis, E.A., Zhang, R.L., Bachmeier, C., Tey, S., Faux, S., Girgis, L., Greenfield, J.R. and Lazarus, S. (2022), JBMR Plus, 6: e10557. https://doi.org/10.1002/jbm4.10557
[7] Cytochromes P450 1A2 and 3A4 Catalyze the Metabolic Activation of Sunitinib. Gracia M. Amaya, Rebecca Durandis, David S. Bourgeois, James A. Perkins, Arsany A. Abouda, Kahari J. Wines, Mohamed Mohamud, Samuel A. Starks, R. Nathan Daniels, and Klarissa D. Jackson. Chemical Research in Toxicology 2018 31 (7), 570-584, https://doi.org/10.1021/acs.chemrestox.8b00005
[8] Interindividual Variability in Cytochrome P450 3A and 1A Activity Influences Sunitinib Metabolism and Bioactivation. Elizabeth A. Burnham, Arsany A. Abouda, Jennifer E. Bissada, Dasean T. Nardone-White, Jessica L. Beers, Jonghwa Lee, Matthew J. Vergne, and Klarissa D. Jackson. Chemical Research in Toxicology 2022 35 (5), 792-806, https://doi.org/10.1021/acs.chemrestox.1c00426
[9] Metabolism of a Bioorthogonal PET Tracer Candidate [19F/18F]SiFA-Tetrazine in Mouse Liver Microsomes: Biotransformation Pathways and Defluorination Investigated by UHPLC-HRMS. Sofia Otaru, Hanna Niemikoski, Mirkka Sarparanta, and Anu J. Airaksinen. Molecular Pharmaceutics 2020 17 (8), 3106-3115, https://doi.org/10.1021/acs.molpharmaceut.0c00523
[10] Probing Mechanisms of CYP3A Time-Dependent Inhibition Using a Truncated Model System. Xiaojing Wang, Minghua Sun, Connie New, Spencer Nam, Wesley P. Blackaby, Alastair J. Hodges, David Nash, Mizio Matteucci, Joseph P. Lyssikatos, Peter W. Fan, Suzanne Tay, and Jae H. Chang. ACS Medicinal Chemistry Letters 2015 6 (8), 925-929, https://doi.org/10.1021/acsmedchemlett.5b00191
[11] Kinesin Spindle Protein (KSP) Inhibitors. 9. Discovery of (2S)-4-(2,5-Difluorophenyl)-N-[(3R,4S)-3-fluoro-1-methylpiperidin-4-yl]-2-(hydroxymethyl)-N-methyl-2-phenyl-2,5-dihydro-1H-pyrrole-1-carboxamide (MK-0731) for the Treatment of Taxane-Refractory Cancer. Christopher D. Cox, Paul J. Coleman, Michael J. Breslin, David B. Whitman, Robert M. Garbaccio, Mark E. Fraley, Carolyn A. Buser, Eileen S. Walsh, Kelly Hamilton, Michael D. Schaber, Robert B. Lobell, Weikang Tao, Joseph P. Davide, Ronald E. Diehl, Marc T. Abrams, Vicki J. South, Hans E. Huber, Maricel Torrent, Thomayant Prueksaritanont, Chunze Li, Donald E. Slaughter, Elizabeth Mahan, Carmen Fernandez-Metzler, Youwei Yan, Lawrence C. Kuo, Nancy E. Kohl, and George D. Hartman. Journal of Medicinal Chemistry 2008 51 (14), 4239-4252, https://doi.org/10.1021/jm800386y
[12] Overcoming Time-Dependent Inhibition (TDI) of Cytochrome P450 3A4 (CYP3A4) Resulting from Bioactivation of a Fluoropyrimidine Moiety. Mihirbaran Mandal, Kaushik Mitra, Diane Grotz, Xinjie Lin, Jairam Palamanda, Pramila Kumari, Alexei Buevich, John P. Caldwell, Xia Chen, Kathleen Cox, Leonard Favreau, Lynn Hyde, Matthew E. Kennedy, Reshma Kuvelkar, Xiaoxiang Liu, Robert D. Mazzola, Eric Parker, Diane Rindgen, Edward Sherer, Hongwu Wang, Zhaoning Zhu, Andrew W. Stamford, and Jared N. Cumming. Journal of Medicinal Chemistry 2018 61 (23), 10700-10708, https://doi.org/10.1021/acs.jmedchem.8b01326
[13] Chemical Aspects of Human and Environmental Overload with Fluorine. Jianlin Han, Loránd Kiss, Haibo Mei, Attila Márió Remete, Maja Ponikvar-Svet, Daniel Mark Sedgwick, Raquel Roman, Santos Fustero, Hiroki Moriwaki, and Vadim A. Soloshonok. Chemical Reviews 2021 121 (8), 4678-4742, https://doi.org/10.1021/acs.chemrev.0c01263